Chronic graft-vs-host disease is a major cause of late, nonrelapse death following allogeneic hematopoietic stem cell transplantation. In addition, chronic graft-vs-host disease results in significant functional impairment and decreased quality of life for long-term survivors of stem cell transplant. The incidence of chronic graft-vs-host disease is rising with wider availability of peripheral blood stem cells as a graft source, but other factors such as prior acute graft-vs-host disease, older transplant recipient age, and male recipients of stem cells from female donors also predispose individuals to the development of chronic graft-vs-host disease.
While the pathophysiology of acute graft-vs-host disease has been described, chronic graft-vs-host disease involves a less understood biologic pathway. The end result is a complex multisystem disorder characterized by immunodeficiency, immune dysregulation and, ultimately, impaired organ function. Previously, the 100-day demarcation was used to delineate acute from chronic graft-vs-host disease. However, in the era of nonmyeloablative hematopoietic stem cell transplantation and common use of donor lymphocyte infusions, this demarcation no longer exists.
Clinical Manifestation
Approximately 60% to 70% of allogeneic stem cell transplant recipients will develop chronic graft-vs-host disease. Nearly one-third of chronic graft-vs-host disease develops de novo, with the remaining two-thirds split evenly among those whose disease occurs as either a continuous progression from acute graft-vs-host disease or after a quiescent period following previous acute graft-vs-host disease. Chronic graft-vs-host disease can be categorized as classic (with only typical chronic skin lesions) or overlap (presence of both acute and chronic cutaneous graft-vs-host disease lesions along with diarrhea and liver dysfunction).
Nearly all cases of chronic graft-vs-host disease involve the skin and/or mucous membranes. This may manifest as oral or conjunctival dryness, dental caries, periodontitis, or gingivitis. Oral lesions may resemble lichen planus, characterized by reticulated white patches or plaques with the ability to ulcerate and cause significant pain and weight loss from anorexia. Ocular lesions may cause dryness, photophobia, and excessive tearing; severe cases can lead to corneal epithelial sloughing and cicatricial conjunctivitis. Vulvovaginal involvement can be associated with urinary and sexual dysfunction.
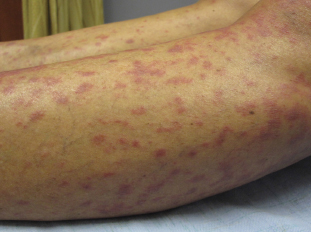
Skin involvement is the hallmark of chronic graft-vs-host disease, and lesions can be classified as either sclerotic or nonsclerotic. Nonsclerotic lesions commonly follow a lichen planus–like morphology (Fig. 1); they are violaceous, flat-topped, and slightly scaly. Sclerotic lesions are indurated, poorly circumscribed, and may appear hyperpigmented.
Progressive sclerotic skin lesions, whether focal or generalized, may result in significant impairment of activities of daily living and deconditioning. Severe sclerosis can lead to involvement of soft tissue and muscle, can cause nerve entrapment, and may ultimately result in chronic skin ulceration (Fig. 2). Loss of skin adnexal structures can lead to permanent alopecia, nail loss, and impairment of sweating. More rare cutaneous morphologies include morbilliform lesions, eczematous forms, and ichthyotic lesions.
Assessment
Unlike acute graft-vs-host disease, there is no standardized grading schema to assess chronic cutaneous graft-vs-host disease. However, a National Institutes of Health (NIH)-developed scoring guide1 assesses the severity of skin lesions based on the amount of body surface area involved along with the presence of sclerotic features. The most severely affected individuals are those with a body surface area > 50% and sclerosis that impairs mobility, causes ulcerations, or results in severe pruritus.
A recently validated grading system to assess oral chronic graft-vs-host disease involvement is based on the presence and extent of erythema, hyperkeratosis, ulceration, and number of mucoceles; patients are stratified as mild, moderate, or severe.2
Treatment Recommendations
For lichen planus–like skin lesions, high potency topical steroids (clobetasol, fluocinonide) applied twice daily and emollients applied after bathing are preferred initial treatment for patients who don’t require systemic treatment, or may be used in conjunction with systemic treatment if indicated. Triamcinolone 0.1% cream used once or twice daily is optimal for maintenance topical therapy. Sclerotic skin lesions respond poorly to topical steroids, though there is some anecdotal evidence supporting the use of calcipotriene cream or ointment as a mechanism to soften sclerotic skin.
For oral lesions, fluocinonide gel or tacrolimus 0.1% ointment can be applied twice daily to lips or mucosal surfaces, including eroded areas. Dexamethasone solution can be swished and spit for oral mucosal lesions, but close observation for the development of candidiasis as a result is warranted. Viscous lidocaine can similarly be used to swish and spit, and may provide pain relief to allow for oral intake of foods and liquids.
Physical therapy to maintain range of motion and strength for patients with sclerotic graft-vs-host disease is vital. Aggressive wound care for sclerotic skin lesions can preclude the development of ulcerations, which, if severe, predispose to serious skin and soft-tissue infections.
Algorithms for first-line systemic treatment of chronic graft-vs-host disease are controversial, though most patients are initiated on prednisone at a dose of 1 mg/kg/d. In many patients, a calcineurin inhibitor is either started at the same time, or during an attempt to taper the steroid dose.
Recent NIH guidelines3 suggest starting systemic treatment if there is severe involvement of one organ, or if three separate organs are involved to any extent. Cyclophosphamide, azathioprine, methotrexate, and sirolimus (Rapamune) are accepted second-line agents for patients that fail systemic steroids; failure is defined as either: (1) progression of chronic graft-vs-host disease despite 2 weeks of systemic steroids at a dose of 1 mg/kg/d, (2) no improvement after 4 to 8 weeks of sustained therapy, or (3) inability to taper steroid dose.
Imatinib (Gleevec) has shown modest benefit for patients with sclerotic graft-vs-host disease, and it is currently under investigation in this setting. Extracorporeal photopheresis has become an additional second-line treatment for chronic graft-vs-host disease patients, and offers potential benefit without further immunosuppression.
Pentostatin, rituximab (Rituxan), thalidomide (Thalomid), mycophenolate mofetil, tumor necrosis factor inhibitors, and alefacept (Amevive) are also used when first-line treatment fails. In addition, sclerotic skin lesions may be amenable to either PUVA (psoralen plus ultraviolet A [UVA]) or UVA1 phototherapy at a dermatologist’s office. ■
Dr. Cotliar is Associate Professor of Dermatology, General Internal Medicine, and Geriatrics at Northwestern University Feinberg School of Medicine, Chicago.
Disclosure: Dr. Cotlier reported no potential conflicts of interest.
References
1. Filipovich AH, Weisdorf D, Pavletic S, et al: National Institutes of Health consensus development project on criteria for clinical trials in chronic graft-versus-host disease: I. Diagnosis and staging working group report. Biol Blood Marrow Transplant 11:945-956, 2005.
3. Perez-Simon JA, Encinas C, Silva F, et al. Prognostic factors of chronic graft-versus-host disease following allogeneic peripheral blood stem cell transplantation: the national institutes health scale plus the type of onset can predict survival rates and the duration of immunosuppressive therapy. Biol Blood Marrow Transplant 14:1163-1171, 2008.
Dermatologic Events in Oncology is guest edited by Mario E. Lacouture, MD, an Associate Member in the Division of Dermatology, Department of Medicine, at Memorial Sloan-Kettering Cancer Center, New York. He is a board-certified dermatologist with a special interest in dermatologic conditions that result from cancer treatments.