
Effective communication with patients and their caregivers about the available evidence is key to successful delivery of integrative medicine interventions.— Gabriel Lopez, MD
Tweet this quote
The ASCO Post’s Integrative Oncology series is intended to facilitate the availability of evidence-based information on integrative and complementary therapies sometimes used by patients with cancer. In this installment, Gabriel Lopez, MD, emphasizes the importance of effective communication and continual symptom assessment for the successful integration of complementary therapies such as acupuncture, mind-body practices, and music into conventional cancer care.
Integrative medicine in the context of oncology care offers unique opportunities to improve disease-related and treatment-related symptoms. According to an expert consensus panel, integrative oncology is defined as “a patient-centered, evidence-informed field of cancer care that utilizes mind and body practices, natural products, and/or lifestyle modifications from different traditions alongside conventional cancer treatments. Integrative oncology aims to optimize health, quality of life, and clinical outcomes across the cancer care continuum and to empower people to prevent cancer and become active participants before, during, and beyond cancer treatment.”1 The aims of integrative oncology align with the palliative care goals of optimizing health and quality of life across the cancer continuum, from diagnosis through advanced disease and into survivorship, helping to manage the late effects of cancer treatment. Major cancer centers across the country now offer integrative medicine as part of palliative or supportive care programs.2
Communication Is Key
One of the challenges in developing an integrative oncology approach to symptom control is in navigating the vast amount of information available through the media, Internet, and community. Some of this information may be unreliable and contribute to patient confusion, leading to uninformed decisions about how to utilize these approaches safely and effectively. An evidence-informed approach, then, is best developed as part of a coordinated effort with the oncology care team and programs such as supportive care, palliative care, and integrative oncology.
Patients who are experiencing a high symptom burden or those with advanced or incurable disease may turn to alternative therapies for controlling both their symptoms and the disease. One survey identified patients with cancer who have distant incurable disease as 11.6 times more likely to use complementary or alternative therapies than are patients who have localized disease.3 Some alternative approaches, such as high-dose antioxidant therapies or herbal supplements, can be harmful through herb-drug interactions, direct organ toxicity, decreased treatment efficacy, or by promoting cancer growth. Effective communication with patients and their caregivers about the available evidence is key to successful delivery of integrative medicine interventions.
Symptom Assessment
There is increasing evidence regarding the benefits of integrative medicine approaches for controlling both physical and psychosocial symptoms associated with cancer and its treatments. An essential component in making decisions about the appropriate interventions that can best help address symptoms is through continual assessment. A physical exam, review of the patient’s cancer history, and understanding comorbid conditions, as well as the routine use of patient-reported outcomes tools to capture self-reported symptoms, can all help with decision-making, identifying baseline symptoms, and tracking progress.
Evidence-Based Recommendations: Interventions
Complementary modalities commonly available to patients fall under the broad categories of natural products, mind-body practices, and whole health systems such as traditional Chinese medicine. The National Comprehensive Cancer Network guidelines currently include a number of integrative approaches as part of recommendations for managing symptoms such as pain, anticipatory nausea/vomiting, fatigue, and overall distress. With regard to mind-body approaches such as acupuncture, meditation, oncology massage, and music therapy, there is moderate to high evidence of their effectiveness in symptom management.4
Guest Editor

Jun J. Mao, MD, MSCE
Integrative Oncology is guest edited by Jun J. Mao, MD, MSCE, Laurance S. Rockefeller Chair in Integrative Medicine and Chief of Integrative Medicine Service at Memorial Sloan Kettering Cancer Center, New York.
Acupuncture has been shown to be effective for relief of pain and nausea, and preliminary data exist for its ability to relieve hot flashes, xerostomia, neuropathy, and headache. Massage was reported to be useful for relieving pain, anxiety, and fatigue, and music therapy may help to manage mood disturbances, including anxiety.4,5 In 2018, ASCO endorsed the Society of Integrative Oncology guidelines on the use of integrative therapies during and after breast cancer treatment.6 The recommendations include the use of meditation for reducing anxiety, alleviating mood disturbance, and improving quality of life. There is also interest in learning more about the potential role of meditation in relieving cancer-related cognitive deficits and that of massage for addressing chemotherapy-induced peripheral neuropathy.
Practice Recommendations
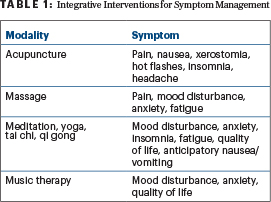
Table 1: Integrative Interventions for Symptom Management
Evidence-informed resources such as clinical practice guidelines can help providers with reliable information regarding the use of complementary approaches. Several frameworks have also been proposed to aid design patient-centered, personalized integrative oncology care plans.7,8 Furthermore, including individuals with expertise in integrative oncology can facilitate identifying complementary therapies that can best address the palliative care needs of patients with cancer. Table 1 lists modalities that can be included as part of a comprehensive approach to help optimize symptom control.
DISCLOSURE: Dr. Lopez reported no conflicts of interest.
REFERENCES
1. Witt CM, Balneaves LG, Cardoso MJ, et al: A comprehensive definition for integrative oncology. J Natl Cancer Inst Monogr 2017(52), 2017.
2. Yun H, Sun L, Mao JJ: Growth of integrative medicine at leading cancer centers between 2009 and 2016. J Natl Cancer Inst Monogr 2017(52), 2017.
3. Richardson MA, Sanders T, Palmer JL, et al: Complementary/alternative medicine use in a comprehensive cancer center and the implications for oncology. J Clin Oncol 18:2505-2514, 2000.
4. Lopez G, Liu W, Milbury K, et al: The effects of oncology massage on symptom self-report for cancer patients and their caregivers. Support Care Cancer 25:3645-3650, 2017.
5. Lopez G, Christie AJ, Powers-James C, et al: The effects of inpatient music therapy on self-reported symptoms at an academic cancer center: A preliminary report. Support Care Cancer 27:4207-4212, 2019.
6. Lyman GH, Greenlee H, Bohlke K, et al: Integrative therapies during and after breast cancer treatment: ASCO endorsement of the SIO Clinical Practice Guideline. J Clin Oncol 36:2647-2655, 2018.
7. Lopez G, Mao JJ, Cohen L: Integrative oncology. Med Clin North Am 101:977-985, 2017.
8. Latte-Naor S, Mao JJ: Putting integrative oncology into practice: Concepts and approaches. J Oncol Pract 15:7-14, 2019.

