Worldwide, the global average surface temperature has risen at a similar rate of 0.17°F per decade since 1901, with the warmest year on record occurring in 2016 and the second warmest occurring in 2020. However, according to NOAA, since the late 1970s, the United States has warmed faster than the global rate.1 Unless ambitious measures are taken to curb climate change, global temperatures are projected to rise by 3°C or more above preindustrial levels by 2100.2 The goals outlined in the Paris Agreement, which the United States rejoined in February, include substantially reducing global greenhouse gas emissions to limit global warming to well below 2°C above preindustrial levels and preferably to 1.5°C.3
The cumulative impact of global warming on the environment can already be seen in the loss of glaciers and polar ice sheets, rising sea levels and warming oceans, and increases in extreme weather events leading to increased storm and flooding intensity and severe heatwaves, droughts, and wildfires—as well as in the rising incidences of cancer. A recent review of the literature chronicling the effect of climate change on chronic diseases, especially cancer, by Robert A. Hiatt, MD, PhD, and Naomi Beyeler, MPH, details how human activities, particularly the burning of fossil fuels, adds carbon dioxide to the atmosphere, setting off a chain reaction of soaring temperatures and creating air pollution from fine particulate matter. The effect of particulate air pollution over the 21st century worldwide, according to the review, will lead to an increase in premature mortality and lung cancer in all regions except Africa. In addition, increased exposure to ultraviolet radiation is leading to a rise in all skin cancers and may be responsible for 76% of new melanoma cases, primarily in North America, Europe, and Oceania.4
Studies are also predicting that rising temperatures and changes in rainfall patterns from climate change will result in increases in food-borne, water-borne, and vector-borne diseases; food insecurity; incidence and severity of asthma and other respiratory diseases; mental health problems; and disruptions in access to and quality of health care for cancer prevention, detection, and management.5

Robert A. Hiatt, MD, PhD

Naomi Beyeler, MPH
In a wide-ranging discussion with The ASCO Post, Dr. Hiatt talked about the vast implications of climate change on cancer; how weather-related disasters will exacerbate inequities in cancer care; and what the oncology community can do to reduce its carbon footprint on the environment. Dr. Hiatt is Professor, Department of Epidemiology and Biostatistics at the University of California San Francisco (UCSF) and Associate Director of Population Sciences at UCSF Helen Diller Family Comprehensive Cancer Center.
Assessing the Impact of Climate Change on Cancer
Your review of the literature on the effect of climate change on cancer incidence and mortality presented a sobering account of how rising temperatures will negate the progress made in the prevention and treatment of cancer globally. How much could climate change increase the incidence and mortality of cancer worldwide?
The precise numbers are difficult to quantify because of the complex interplay of climate change exposures and outcomes over time, multiple confounding factors, and the challenges of establishing causal relationships. The studies on which our review is based are predictions of exposures from air pollution and ultraviolet radiation that are currently occurring and what the estimated effects of these exposures may be in the future. We supplemented our review with additional literature that explored the specific pathways from climate change to cancer, but it is not the same as conducting a traditional epidemiologic study in which you have some sort of comparison groups.
Rather than make a guess at what the precise impact of climate change on cancer may be, it is best for us to understand that environmental determinants on cancer are already with us, and we need to be aware of them, collect more data, and make investments in combating climate change.
What will be the impact of climate change and cancer on low- and middle-income countries compared with high-income countries?
Cancer care and control systems are already tenuous in low- and middle-income countries, where access to basic cancer screenings (including for early detection of cervical cancer) and cancer treatment is low or nonexistent. The disruption in peoples’ lives brought about by extreme weather events like drought and flooding will likely make cancer care even less of a high priority in low-resource countries.
In other words, although a lot of work has been done in these countries to establish systems to treat cancer and educate the public about how to prevent cancer and detect it early, it won’t take much to disrupt that whole fragile system of health care caused by climate change.
REDUCING THE CARBON FOOTPRINT OF CANCER CARE
It is becoming increasingly clear from studies published over the past year of the direct relationship between the environmental effects from climate change and the risk they pose for the development of cancer, disruptions to care, and survival. In a commentary written by Leticia M. Nogueira, PhD, MPH, Senior Principal Scientist, Health Services Research at the American Cancer Society, and her colleagues, titled “Climate Change and Cancer,” in the July/August 2020 issue of CA: A Cancer Journal for Clinicians, the authors presented some contributions of greenhouse gas emissions made by cancer care and how they may be reduced.
Impact of Cancer Mortality on Changes in the Food Supply
Increasing temperatures, flooding, drought, and hurricanes are affecting the quality and quantity of food production, and rising ocean temperatures are threatening the world’s fisheries. Please talk about how changes in the food supply and food scarcity might increase the incidence of cancer.
The best data we have on nutrition and cancer show that there is an overall protective benefit of eating a healthy diet of whole grains, fish, fruits, and vegetables and limiting red meat and processed meat consumption, especially for reducing the risk of colorectal and breast cancers. Extreme weather events, higher ground-level ozone, declines in pollinators such as honey bees, and sea-level rise all negatively affect food production and crop yields. Modelling studies of chemical pollutants in glacial meltwater in the Alaskan Arctic and the Swiss Alps have shown elevated concentrations of persistent organic pollutants that can accumulate in the local fish supply and might increase the lifetime cancer risk among people consuming high amounts of fish.
Although the exact overall effects of climate change on nutrition-related cancers are difficult to determine, a modeling study predicted there would be 534,000 climate-related deaths worldwide, including deaths from cancer, by 2050, from changes in the food supply and the reduced consumption of fruits and vegetables.6
In general, you can imagine how disruptions in the food supply will result in people not having enough healthy foods to consume, which will lead to multiple negative health outcomes, including the development of cancer.
Studies have shown that the biggest contributors to the carbon footprint in the U.S. health-care system are the hospital and pharmaceutical industry sectors.— Robert A. Hiatt, MD, PhD
Tweet this quote
Overcoming Disruptions in Health Care
Preventive screenings for breast, cervical, and colon cancers plummeted by between 86% and 94% during the first four months of 2020 due to the COVID-19 pandemic.7 As a result of delayed screenings and care, the National Cancer Institute is predicting that an additional 10,000 deaths from breast and colorectal cancers will occur over the next decade.8 Your review found that disruptions in hospital functioning caused by weather disasters like hurricanes can result in substantial delays in oncology treatment. Please talk about how extreme weather events affect cancer treatment and survival.
We wrote our article at the beginning of the COVID-19 pandemic, anticipating the parallel of disruptions in a fragile health-care system brought on by the pandemic and what could happen from health-care disruptions caused by climate change. One of the most powerful impressions I was left with during our research was, as sophisticated as we are in medicine, we had tremendous challenges in coping with COVID.
We saw major disruptions in hospital functioning and delays in oncology treatment due to damaged hospital infrastructures during several hurricanes over the past 2 decades, including Hurricane Katrina in 2005. The damage to the health-care facilities in New Orleans and the surrounding cities reduced access to cancer care for years after the disaster. In our study, we found that the 10-year survival for breast cancer was lower for people affected by the hurricane compared with those who had not been affected by Katrina. A systematic review of natural disasters and cancer found evidence of higher cancer mortality after these disasters than before these weather events.
If climate change adds to the frequency of pandemics and severe weather events, how are we going to ensure the delivery of uninterrupted complex oncology care for patients in an already fragile and fragmented health-care system?
Exacerbating the Inequities in Cancer Care
Racial and ethnic minorities already experience more aggressive cancers and worse survival outcomes than White patients. How might climate change exacerbate cancer outcome disparities for minority patients?
Those at the bottom of the socioeconomic ladder always sustain the worst effects from any threat—whether it be COVID-19, food and housing shortages, or climate change.
Those at the bottom of the socioeconomic ladder always sustain the worst effects from any threat—whether it be COVID-19, food and housing shortages, or climate change.— Robert A. Hiatt, MD, PhD
Tweet this quote
The least privileged and most disadvantaged in our society, including racial and ethnic minorities, persons of lower socioeconomic status, people with disabilities, LGBTQ (lesbian, gay, bisexual, transgender, and queer/questioning) populations, and new immigrants, always sustain the worst effects of health inequities. Whenever there is a threat, such as a pandemic or a hurricane, the gaps between those who can deal with the threat and receive high-quality health care and those who are not able to access care become even greater. I expect the inequities that we see in cancer outcomes will be made worse by climate change and the health-care threats associated with it.
Mitigating the Impact of Climate Change on Cancer Care
What can be done to fortify the health-care system to mitigate the impact of climate change on cancer care?
There needs to be high-level thinking from public health-care professionals and political leaders about how to anticipate the environmental crises caused by climate change that are likely to come and what policies could be put in place to minimize health-care risks. We have not seen the last global pandemic. We have not seen the last wildfire in California. We have not seen the last hurricane in New Orleans or New York City. The Arctic ice cap is melting. There will be future challenges we have to face. We need to prepare climate-resilient health-care systems to ensure continuity of care during climate-related events.
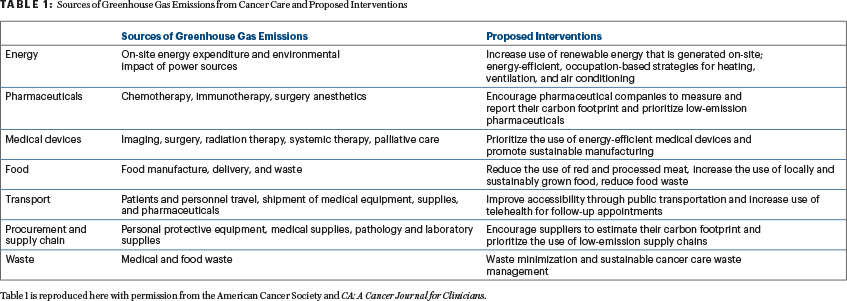
Opportunities exist for changes in policies within energy, agriculture, transportation, health care, and other sectors to substantially reduce greenhouse gas emissions (Table 1), slow climate change, and avoid extreme fluctuations in temperature that can reduce the risk of cancer and other health conditions. Although the time to implement these changes is now, it is difficult to do so because many political leaders and other decision-makers do not want to invest in mitigation efforts for future events that might happen, so efforts are not made in long-term climate action planning.
Forty years ago, the alarm on climate change was sounded, and it was ignored. During the early lockdown response to the COVID-19 pandemic, we saw a striking reduction in air pollution, showing how extreme measures, if systematically organized and mandated, can result in rapid environmental change.
We need to learn the lessons from the current pandemic and see how we can apply them to meet the global challenge of climate change. These lessons include the need for investments in public health and health-care infrastructure, research, and intense collective action on improving global health care.
Reducing Oncology’s Footprint on the Environment
Cancer care—including chemotherapy, immunotherapy, and surgery anesthetics; imaging devices; and radiation therapy equipment—contributes to greenhouse gas emissions and climate change. What can the oncology community do to reduce the oncology footprint on the environment?
Studies have shown that the biggest contributors to the carbon footprint in the U.S. health-care system are the hospital and pharmaceutical industry sectors, so optimizing operating room ventilation based on occupancy and demand and using more energy-efficient computed tomography and magnetic resonance imaging machines can help to reduce greenhouse gas emissions.9 Thinking about how to use energy in a more sustainable way throughout the health-care system—for example, by avoiding duplication in cancer care follow-up from multiple oncology subspecialties and primary care; enacting policies to increase public transportation and encourage walking or cycling to cancer centers; and utilizing telehealth for cancer appointments when possible—can all help to reduce the environmental impact on climate change.
In addition, the oncology community can support ways to reduce the cancer risks associated with climate change; advocate for the development of new climate policies in their communities; encourage implementation of current ones, such as the goals outlined in the Paris Agreement; and undertake research and education on climate change and health.
DISCLOSURE: Dr. Hiatt reported no conflicts of interest.
REFERENCES
1. United States Environmental Protection Agency: Climate Change Indicators: U.S. and Global Temperatures. Available at www.epa.gov/climate-indicators/climate-change-indicators-us-and-global-temperature#ref1. Accessed July 6, 2021.
2. Climate Action Tracker: Temperatures: 2100 Warming Projections. Available at https://climateactiontracker.org/global/temperatures/. Accessed July 6, 2021.
3. United Nations Climate Change: The Paris Agreement. Available at https://unfccc.int/process-and-meetings/the-paris-agreement/the-paris-agreement. Accessed July 6, 2021.
4. Hiatt RA, Beyeler N: Cancer and climate change. Lancet Oncol 21:e519-e527, 2020.
5. Schiller JH, Averbuch SD, Berg CD: Why oncologists should care about climate change. JCO Oncol Pract 16:775-778, 2020.
6. Springmann M, Mason-D’Croz D, Robinson S, et al: Global and regional health effects of future food production under climate change: A modelling study. Lancet 387:1937-1946, 2016.
7. Epic Health Research Network: Cancer Screenings Are Still Lagging. June 9, 2021. Available at https://ehrn.org. Accessed July 6, 2021.
9. Nogueira LM, Yabroff KR, Bernstein A: Climate change and cancer. CA Cancer J Clin 70:239-244, 2020.

